Summary
Protein energy malnutrition (PEM) affects millions of children across India, especially in rural and marginalised communities. PEM develops when children do not receive enough protein and calories to support normal growth and development.
This condition weakens immunity, delays physical and cognitive growth, and increases the risk of infections. Severe PEM can be life-threatening if left untreated. By understanding protein energy malnutrition (PEM), its causes, symptoms, and prevention strategies, carers and communities can take effective steps to protect children’s health.
What is Protein Energy Malnutrition?
Protein energy malnutrition is a serious form of undernutrition. It occurs when children consistently consume insufficient protein and calories.
- Protein supports muscle development, immune defence, and tissue repair.
- Energy (calories) fuels daily activities, organ function, and growth.
Without these essential nutrients, the body begins to break down its own tissues, leading to severe health complications. Children under five years old are most at risk.
How PEM Affects Children
PEM has immediate and long-term effects on children’s health:
- Stunted growth: Children fail to reach expected height and weight.
- Delayed cognitive development: Malnutrition slows learning and memory.
- Weakened immunity: Frequent infections like diarrhoea, pneumonia, and intestinal worms occur.
- Life-threatening complications: Severe PEM can lead to organ failure or death.
Early detection and intervention can reverse many of these effects.
What Are the Main Causes of PEM?
PEM results from a combination of dietary, health, and socioeconomic factors.
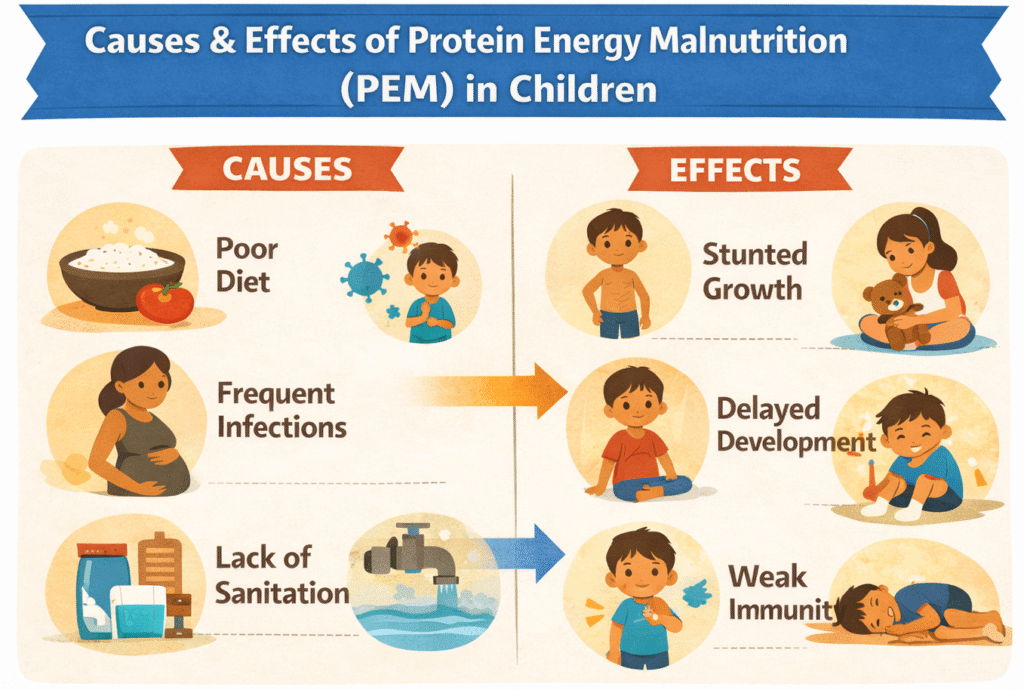
- Poor Dietary Intake
Children often eat diets heavily based on cereals with inadequate protein sources like pulses, dairy, eggs, or meat. Poverty and food insecurity make this problem worse. - Repeated Infections
Frequent infections reduce nutrient absorption, lower appetite, and increase energy needs. This creates a vicious cycle: malnutrition increases infection risk, and infections worsen malnutrition. - Inadequate Sanitation and Hygiene
Unsafe water and poor sanitation expose children to diseases, worsening malnutrition. - Maternal Undernutrition
Undernourished mothers are more likely to give birth to low birth weight babies. These infants are at higher risk of PEM during early childhood.
Types of Protein Energy Malnutrition
Protein Energy Malnutrition (PEM) appears in three main forms:
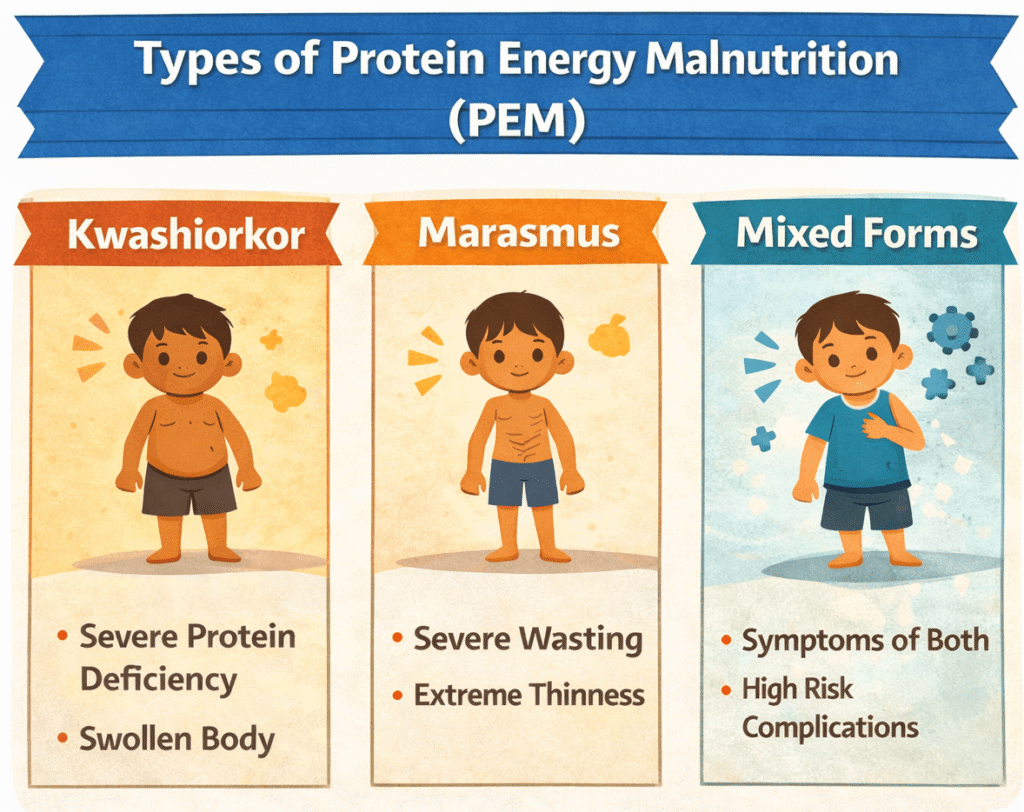
- Kwashiorkor
Severe protein deficiency, sometimes with adequate calories.
Symptoms: Swelling of limbs and face, thinning hair, skin changes, and enlarged liver.
Immediate medical attention is required. - Marasmus
Severe deficiency of both protein and calories.
Symptoms: Extreme thinness, visible bones, muscle wasting, weakness. - Mixed Forms
Children show characteristics of both kwashiorkor and marasmus. These cases have the highest risk of complications and death.
Signs and Diagnosis of Protein Energy Malnutrition
Early identification saves lives. Carers should watch for:
- Poor weight gain
- Thin body and visible bones
- Swelling of limbs or face
- Frequent infections
- Fatigue or lethargy
- Delayed developmental milestones
Doctors diagnose PEM using:
- Weight-for-age and height-for-age charts
- Mid-upper arm circumference (MUAC)
- Dietary history assessment
- Laboratory tests if needed
Preventing Protein Energy Malnutrition
Communities and families can prevent PEM through simple, practical steps:
- Exclusive breastfeeding: For the first six months of life.
- Balanced complementary feeding: Introduce protein-rich foods such as pulses, dairy, eggs, and vegetables after six months.
- Clean water and sanitation: Reduce infection risk.
- Nutrition education: Teach caregivers about healthy feeding practices and early warning signs.
How BXI Foundation Tackles Protein Energy Malnutrition

At BXI Foundation, we implement sustainable programmes to reduce child malnutrition:
- Conduct community nutrition awareness campaigns
- Organise growth monitoring camps
- Support kitchen garden initiatives in households and schools
- Provide school-based nutrition drives
- Train women and local health workers
Role of Kitchen Gardens in Preventing Protein Energy Malnutrition
Kitchen gardens provide:
- Fresh vegetables and fruits year-round
- Affordable, nutrient-rich foods
- Dietary diversity for children and families
- Empowerment for women and local communities
By growing their own produce, families reduce dependency on markets, improve nutrition, and create long-term health benefits.
Early Intervention Saves Lives
Early treatment reverses PEM in most children. Action steps include:
- Therapeutic feeding programs
- Medical supervision
- Infection control and vaccinations
- Regular growth monitoring
Delayed intervention increases the risk of permanent developmental problems.
Bottom Line
Protein Energy Malnutrition is preventable and treatable. Early detection, proper nutrition, and community support can protect children from serious health risks.
BXI Foundation is committed to ensuring every child receives adequate nutrition, grows healthily, and thrives in life. Support our programs today to help children stay healthy, learn better, and reach their full potential.

